Dr Abhijeet G. Shinde, DNB (Internal Medicine)
Physician • Author • Medical Philosopher
Founder, The Thinking Healer™
Abstract
Clinical medicine operates under persistent epistemic uncertainty despite unprecedented advances in diagnostic technology, biomedical data generation, and algorithmic assistance. Diagnostic error continues to arise from interacting cognitive, systemic, and contextual factors.
Among these, premature cognitive closure and unexamined assumptions remain central and modifiable determinants of clinical failure. This article advances the argument that structured scepticism—defined as disciplined, methodological doubt directed toward one’s own diagnostic reasoning—functions as a meta-regulatory cognitive strategy within clinical decision-making.
Drawing from philosophical fallibilism, Bayesian epistemology, and contemporary cognitive psychology, the Sceptical Clinical Loop is proposed as an operational framework translating epistemological principles into bedside reasoning practices. Rather than replacing existing models, structured scepticism is positioned as a supervisory mechanism that sustains adaptive reasoning, probabilistic judgement, and diagnostic safety.
1. Introduction: Medicine as an Epistemic Practice
Clinical medicine is fundamentally an epistemic enterprise. Physicians are required to generate actionable judgements under conditions of incomplete information, biological variability, and temporal urgency.
Diagnosis therefore represents the formation of a provisionally justified belief rather than the discovery of absolute truth. Large diagnostic safety studies demonstrate that error emerges not only from lack of knowledge but also from failures in reasoning regulation, communication breakdowns, workflow pressures, and system constraints.
Within this landscape, cognitive biases such as anchoring, availability bias, and premature closure exert substantial influence on diagnostic outcomes. The challenge for modern medicine is therefore not solely acquiring knowledge but governing confidence appropriately in uncertain environments.
2. Philosophical Foundations of Clinical Scepticism
Philosophical scepticism has historically served as a constructive methodological discipline. Cartesian doubt sought clarity through systematic questioning, while Popperian fallibilism emphasised falsification as the engine of scientific progress. Clinical reasoning mirrors these traditions.
Diagnostic hypotheses emerge as tentative explanatory models that must remain revisable. Bayesian epistemology further formalises this principle by demonstrating that belief strength must evolve dynamically with incoming evidence.
Clinical scepticism differs from radical philosophical scepticism; it does not deny knowledge but regulates certainty, ensuring that belief remains proportionate to evidence.
3. Scepticism as Meta-Regulation of Clinical Reasoning
Contemporary theories of clinical reasoning—including Dual Process Theory, illness scripts, and hypothetico-deductive reasoning—describe mechanisms of hypothesis generation. However, these models incompletely address how clinicians monitor and recalibrate their reasoning processes in real time.
Structured scepticism operates at a metacognitive level, supervising both intuitive pattern recognition and analytical deliberation. This regulatory function enables clinicians to revisit assumptions, detect discordant evidence, and prevent stabilisation of incorrect diagnostic frames.
4. The Sceptical Clinical Loop
The Sceptical Clinical Loop operationalises epistemic regulation through an iterative reasoning cycle:
1. Hypothesis Formation : Initial pattern recognition generates diagnostic possibilities.
2. Active Disconfirmation : Intentional search for contradictory data challenges early assumptions.
3. Base-Rate Recalibration : Epidemiological context and patient-specific probability are integrated.
4. Bayesian Updating : Diagnostic likelihood evolves continuously as evidence accumulates.
5. Diagnostic Pause : Explicit acknowledgement of residual uncertainty prior to commitment.
This loop reinforces adaptive reasoning and interrupts premature diagnostic closure (Figure 1).
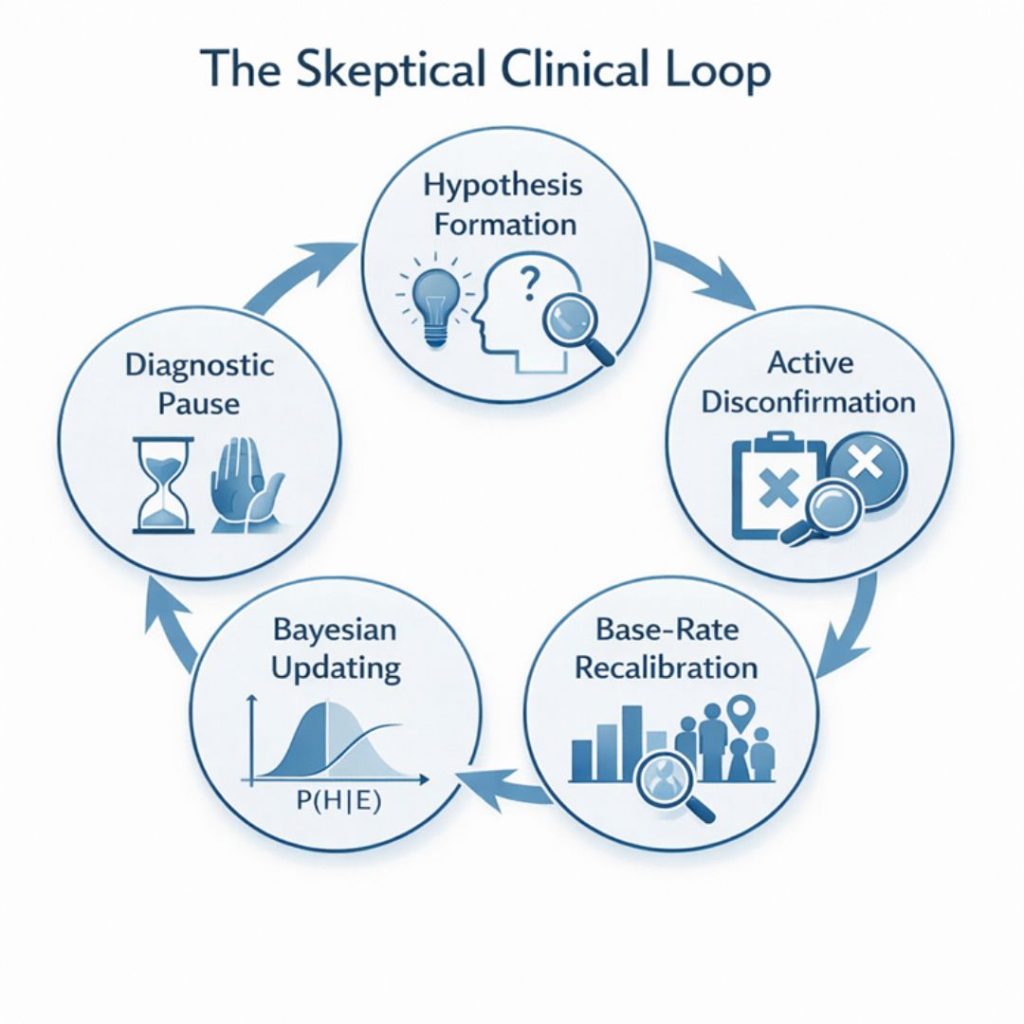
Figure 1. The Sceptical Clinical Loop: A meta-regulatory framework illustrating iterative clinical reasoning through hypothesis generation, active disconfirmation, probabilistic recalibration, Bayesian updating, and diagnostic pause.
5. Clinical Illustrations
Case 1:
Sepsis Mimic — Failure to improve despite appropriate antimicrobial therapy prompted diagnostic reconsideration leading to identification of thyroid storm, illustrating how treatment non-response should trigger epistemic reassessment.
Case 2:
Incidentaloma Cascade — Detection of an adrenal incidentaloma resulted in escalating investigations despite low malignancy probability, demonstrating distortion of judgement when probabilistic scepticism is absent.
Case 3:
Recurrent Pneumonia — Repeated antibiotic treatment obscured hypersensitivity pneumonitis until environmental exposure history was reconsidered.
6. Educational Implications
Medical education has traditionally emphasised knowledge accumulation rather than epistemic discipline. Incorporation of structured scepticism into curricula may include diagnostic pauses, assumption auditing, cognitive autopsy following error, simulation-based reflective training, and explicit teaching of uncertainty tolerance.
7. Toward a Logic of Medical Knowing
Clinical knowledge enables action despite uncertainty rather than elimination of uncertainty itself. Within this framework, scepticism functions as a necessary but not sufficient safeguard complementing expertise, pattern recognition, and evidence synthesis.
Conclusion
Structured scepticism moderates diagnostic confidence, mitigates cognitive bias, and sustains adaptive reasoning under uncertainty. Medicine advances not only through the accumulation of knowledge but also through disciplined methods for questioning its application.
References
1. National Academies of Sciences, Engineering, and Medicine. Improving Diagnosis in healthcare. Washington, DC: National Academies Press; 2015.
2. Graber ML, Franklin N, Gordon R. Diagnostic error in internal medicine. Arch Intern Med. 2005;165(13):1493–1499.
3. Croskerry P. The importance of cognitive errors in diagnosis and strategies to minimize them. Acad Med. 2003;78(8):775–780.
4. Schiff GD, Hasan O, Kim S, et al. Diagnostic error in medicine: analysis of 583 physician-reported errors. Arch Intern Med. 2009;169(20):1881–1887.
5. Kassirer JP. Diagnostic reasoning. Ann Intern Med. 1989;110(11):893–900.
6. Kahneman D. Thinking, Fast and Slow. New York: Farrar, Straus and Giroux; 2011.
7. Elstein AS, Shulman LS, Sprafka SA. Medical Problem Solving: An Analysis of Clinical Reasoning. Cambridge, MA: Harvard University Press; 1978.
8. Norman G. Research in clinical reasoning: past history and current trends. Med Educ. 2005;39(4):418–427.
9. Trowbridge RL, Rencic JJ, Durning SJ. Teaching clinical reasoning. J Hosp Med. 2013;8(10):550–555.
10. Mamede S, Schmidt HG, Rikers RMJP. Diagnostic errors and reflective practice in medicine. J Gen Intern Med. 2007;22(10):1383–1387.
11. Popper KR. The Logic of Scientific Discovery. London: Routledge; 1959.
12. Descartes R. Meditations on First Philosophy. Paris; 1641.












Leave a Reply