Dr. Abhijeet G. Shinde, DNB (Internal Medicine) Physician, Author, and Medical Philosopher Founder, The Thinking Healer
How mathematical logic, Vedantic philosophy, and clinical medicine converge upon a single epistemic method through the universal principle of structured negation
Mathematics · Vedānta · Medicine · Epistemology
ABSTRACT
Diagnostic reasoning in medicine has long been understood as a process of hypothesis generation and systematic elimination. This paper proposes that such reasoning instantiates a universal epistemic structure shared across three distinct intellectual traditions: the double negation principle in formal logic, the neti neti method of Advaita Vedānta, and the differential diagnosis of clinical medicine. Drawing on the philosophy of Karl Popper, the mathematics of Frege and Russell, and the Upanishadic tradition as articulated by Ādi Śṅkarācārya, we present the Medisophy Framework—a three-stage model progressing from negation (neti neti) through discrimination (viveka) to clinical wisdom (prajñā). We further propose five foundational epistemic laws of diagnosis arising from this synthesis and discuss implications for medical education and diagnostic training.
Keywords: clinical reasoning, epistemology, differential diagnosis, Vedānta, falsificationism, medical education, Medisophy
I · INTRODUCTION
Uncertainty and the Architecture of Knowing
The epistemic problem of diagnosis
Every physician who stands at a bedside confronts the same fundamental problem that has occupied logicians, mathematicians, and philosophers across millennia: how does one arrive at truth in conditions of radical uncertainty?
The standard account of diagnosis—history, examination, investigation, and conclusion—is procedurally adequate but epistemologically impoverished. It describes the sequence of clinical reasoning without explaining its underlying logic. What cognitive operation does the physician actually perform? By what mechanism does uncertainty contract into a working diagnosis sufficient to guide action?
We propose that diagnosis enacts a universal epistemic structure best illuminated by placing three traditions in conversation: the formal logic of Frege and Russell, the Advaita Vedānta of the Brihadaranyaka Upanishad as systematized by Śṅkarācārya, and the philosophy of science of Karl Popper. All three locate truth not in accumulation but in the disciplined elimination of the false. All three hold that what survives negation has earned the right to be believed. This convergence is the Medisophy Framework.
II · MATHEMATICAL LOGIC
The Arithmetic of Negation
After Frege, Russell, and the foundations of formal logic
Formal logic establishes, at its most fundamental level, that the systematic removal of negation is a generative act. Negation, fully and consistently applied, yields affirmation. This is not a curiosity of notation — it is a structural property of truth itself.
|
DOUBLE NEGATION ELIMINATION ¬(¬P) ≡ P In classical propositional logic, the double negation of any proposition P is logically equivalent to P. Removing two negations does not merely return to the origin — it confirms and restores the affirmative. |
|
ARITHMETIC ANALOG (−a) × (−b) = ab where a, b > 0 The product of two negative quantities yields a positive result — a consequence not of convention but of the requirement that arithmetic remain internally consistent under the field axioms. |
Gottlob Frege’s Begriffsschrift (1879) formalised the notation of logical negation, and Bertrand Russell’s subsequent work demonstrated that the laws of thought themselves depend upon such structural regularities. The double negation law is not a special case — it is foundational. The epistemological implication is consequential: negation applied with rigour and completeness is not destructive but productive. What remains after all valid negations have been discharged is not emptiness — it is the logically irreducible affirmative.
III · VEDANTIC EPISTEMOLOGY
Neti Neti
Brihadaranyaka Upanishad · Ādi Śṅkarācārya · Advaita Vedānta
Millennia before Frege systematised logical negation, the Upanishadic tradition had independently arrived at the same epistemic architecture. In the Brihadaranyaka Upanishad (c. 700 BCE), the sage Yājñavalkya describes the method by which ultimate reality — Brahman — may be approached. The method is not assertion. It is elimination.
Neti neti — not this, not this. Every proposed identification of the self, of reality, of consciousness is examined and found insufficient. The inquiry proceeds by stripping away every false candidate until what cannot be negated remains.
| नेति | Not the body — the body is contingent, changing, observed; the observer is not what it observes |
| नेति | Not the senses — perception is variable and conditioned; awareness itself is not among its contents |
| नेति | Not the mind — thought arises and dissolves within awareness; the witness of thought is not thought |
| What survives every negation is Ātman — the undeniable, un-negatable remainder |
Ādi Śṅkarācārya’s Advaita systematisation makes explicit what the earlier texts imply: the un-negatable is not what remains by default, but what is revealed as irreducibly real by the very failure of negation to succeed against it. The residue of elimination is not accidental — it is ontologically privileged. The parallel with double negation is not metaphorical. In both traditions, the structural logic is identical: successive elimination purifies the inquiry until the truth, which was present throughout, becomes unavoidable.
IV · CLINICAL REASONING
The Differential as Structured Negation
After Karl Popper · Croskerry · Norman
The physician at the bedside performs, without naming it, an ancient philosophical operation. Faced with a constellation of symptoms, she does not begin with the answer — she begins with a structured field of candidates and subjects each to the pressure of evidence.
Consider the canonical presentation: a 58-year-old with acute chest pain, diaphoresis, and dyspnoea. The differential diagnosis is a discipline of negation:
| Excluded | Myocardial infarction — ECG without ischaemic change; serial troponins within normal range |
| Excluded | Pulmonary embolism — Wells pre-test probability low; D-dimer non-elevated |
| Excluded | Tension pneumothorax — breath sounds bilaterally equal; trachea central; haemodynamics preserved |
| Excluded | Aortic dissection — pain character atypical; pulse deficits absent; chest radiograph unremarkable |
| What evidence cannot exclude becomes the working diagnosis — sufficient to guide therapeutic action |
Karl Popper’s philosophy of science provides the theoretical scaffolding for this clinical practice. In The Logic of Scientific Discovery (1934), Popper argued that no finite number of confirming observations can establish a hypothesis as true, but a single disconfirming observation can establish it as false. Knowledge advances through falsification rather than verification. Clinical diagnosis is applied Popperian epistemology: the physician does not accumulate evidence until certainty is achieved — certainty is never achieved. She eliminates until the remaining explanation is more defensible than any alternative, and acts upon it. As Croskerry (2009) and Norman (2009) have demonstrated, diagnostic error correlates not with insufficient data collection but with failures of this eliminative process — anchoring upon an early hypothesis, or failing to generate an adequate differential in the first place.
V · FIGURE 1
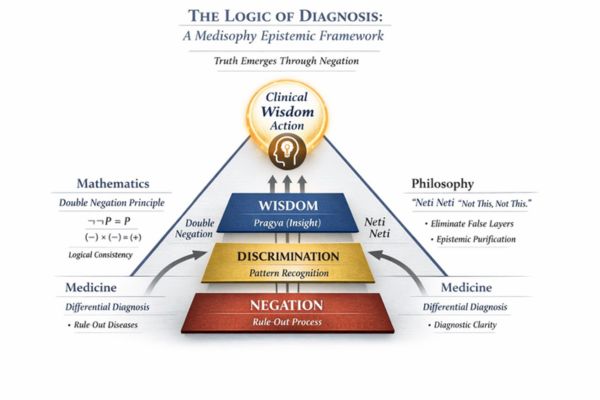
The Medisophy Epistemic Framework
Conceptual diagram with cross-domain annotations
| THE MEDISOPHY EPISTEMIC FRAMEWORK · FIGURE 1 | ||
| STAGE III ◎ CLINICAL WISDOM Prajñá Therapeutic Decision · Phronēsis | STAGE II ◈ DISCRIMINATION Viveka Pattern Recognition · Probabilistic Reasoning | STAGE I ∅ NEGATION Neti Neti Differential Diagnosis · Falsification |
| ↑ Negation contracts uncertainty → Discrimination weighs survivors → Wisdom enacts judgment ↑ | ||
| MATHEMATICS ¬(¬P) ≡ P | VEDĀNTA Neti Neti · Viveka · Prajñá | MEDICINE Falsification · Differential · Phronēsis |
|
FIGURE 1 LEGEND · JOURNAL FORMAT Figure 1. The Logic of Diagnosis: A Medisophy Epistemic Framework. Clinical reasoning is conceptualised as a three-stage epistemic progression structured around systematic negation. The upward directionality reflects progressive contraction of diagnostic uncertainty. |
VI · SYNTHESIS
The Epistemic Convergence
A comparative analysis across four traditions
Three traditions, separated by centuries and continents, arrived independently at the same architecture of knowing. The parallel is not rhetorical — it is structural. Each tradition identifies the same epistemic movement: proposal, examination, elimination, residue.
| DOMAIN | THE OPERATION | THE RESIDUE | EPISTEMIC STATUS |
| Mathematics | ¬(¬P) ≡ P | P — the logically affirmative | Necessary truth; the un-negatable is certain |
| Vedānta | Neti neti — systematic elimination | Ātman — the irreducible self | Ontological certainty; the un-negatable is real |
| Popper | Falsificationism — hypothesis elimination | The surviving hypothesis | Provisional warrant; the un-falsified is credible |
| Medicine | Differential diagnosis — systematic rule-out | The working diagnosis | Actionable warrant; sufficient to guide therapeutic decision |
One distinction deserves acknowledgement. Where mathematics and Vedānta aim at certainty, medicine aims at actionable warrant under irreducible uncertainty. The physician does not achieve truth in the logical or metaphysical sense; she achieves a diagnosis defensible enough to act upon. Popperian epistemology bridges this gap precisely: the clinician, like the scientist, cannot verify but must act, and does so on the basis of the hypothesis that has survived the most rigorous available attempt at disproof.
VII · ORIGINAL CONTRIBUTION
The Five Epistemic Laws of Diagnosis
A signature Medisophy framework — structural laws of clinical knowing
From the convergence of these traditions, we derive five foundational epistemic laws governing the logic of clinical diagnosis. These are not empirical generalisations — they are structural features of how diagnosis, as an epistemic practice, must operate to be coherent.
| I |
THE LAW OF RESIDUAL TRUTH Veritas per exclusionem What cannot be excluded must be taken seriously. The working diagnosis is not chosen — it survives. Its warrant derives entirely from the failure of elimination to succeed against it. A diagnosis that has not survived serious attempts at refutation has not earned its standing. |
| II |
THE LAW OF NECESSARY BREADTH Differentia ante exclusio A diagnosis can only survive elimination if it was first included in the differential. Diagnostic error most frequently originates not in faulty reasoning but in an incomplete field of candidates. The hypothesis never generated cannot be the one that survives. Adequate negation requires adequate initial breadth. |
| III |
THE LAW OF ASYMMETRIC STAKES Non excludere periculosa prius Elimination must be ordered by consequence, not by probability alone. The dangerous diagnosis — the one that kills if missed — must be excluded first, even when its prior probability is low. The logic of the differential is not purely Bayesian; it is also ethical. To diagnose without first excluding the lethal alternative is a failure of clinical duty, not merely of statistical reasoning. |
| IV |
THE LAW OF PROVISIONAL COMMITMENT Agere sub incertitudine Clinical action cannot await certainty, for certainty does not arrive. The physician must act upon the most defensible hypothesis available, while remaining genuinely open to revision when new evidence emerges. This is not intellectual weakness — it is the correct epistemic posture when action under uncertainty is morally required. The working diagnosis is explicitly provisional; its provisional character does not diminish its clinical authority. |
| V |
THE LAW OF ENACTED WISDOM Prajñá in actu The final movement of diagnosis exceeds both logic and probability. Clinical wisdom — prajñā — integrates evidence, pattern, experience, and the irreducibly individual context of the patient into a judgment that cannot be fully formalised. This is Aristotle’s phronēsis: practical wisdom that knows not merely what is true in general but what this particular situation requires. No algorithm produces it. It is cultivated across years of practice and failure and care. |
VIII · DISCUSSION
Implications for Medical Education
From framework to pedagogy
The Medisophy Framework carries practical implications for how clinical reasoning is taught, assessed, and developed across the arc of medical training.
|
◈ CURRICULUM DESIGN Medical curricula should explicitly teach the logic of elimination, not merely the content of differentials. Students who understand why the differential operates as structured negation are better positioned to apply this logic to novel presentations they have never previously encountered. |
∅ DIAGNOSTIC ERROR REDUCTION Croskerry’s taxonomy of cognitive bias is enriched by the Medisophy analysis. Anchoring — premature closure on an early hypothesis — is, in epistemic terms, a failure to complete the eliminative process. Teaching students to name this failure philosophically may make it more visible and more corrigible. |
|
◎ ASSESSMENT OF CLINICAL WISDOM Current assessments adequately probe factual knowledge (Stage I) and analytical reasoning (Stage II). The model draws attention to the relative neglect of prajñā-level assessment — the judgment integrating evidence with the particular patient — and invites development of assessment methods adequate to this level. |
∴ INTELLECTUAL SELF-UNDERSTANDING The demonstration that clinical reasoning shares its deep logic with mathematical proof and Vedantic inquiry expands clinicians’ intellectual self-understanding. A physician who recognises herself as performing a practice with roots in Frege and Śṅkarācārya may bring to that practice a richer sense of its philosophical dignity and structural requirements. |
Thomas Kuhn’s observation that paradigm shifts occur when anomalies accumulate that existing frameworks cannot absorb applies with particular force here. The dominant paradigm of medical education — competency-based, procedurally defined, assessment-driven — has generated its own anomaly: physicians who can pass examinations but cannot reason under genuine uncertainty. The Medisophy Framework does not replace this paradigm; it supplies it with the epistemological foundation it currently lacks.
CLOSING STATEMENT · MEDISOPHY FORMULATION
“ Diagnosis is rarely the immediate discovery of truth; it is the disciplined removal of falsehoods until the remaining explanation becomes sufficiently coherent to guide action. What the physician cannot exclude, she must take seriously. What survives every serious attempt at refutation has earned the right to be believed — and, for the patient’s sake, to be acted upon, under the full weight of clinical responsibility. — The Medisophy Formulation |
IX · PRACTICAL AND CLINICAL APPLICATIONS
From Framework to Bedside
Operational translation of the three-stage epistemic model
A framework that cannot be used at the bedside remains a philosophical curiosity. The Medisophy model is not merely descriptive—it is actionable. The three stages map directly onto clinical behaviours that can be taught, observed, assessed, and improved. What follows translates the epistemic architecture of Section VI into concrete protocols, decision tools, and teaching practices suitable for clinical deployment.
The Medisophy Bedside Protocol
A structured clinical checklist applying the three-stage framework
The following protocol operationalises the three Medisophy stages as a disciplined sequence of explicit clinical questions. It is not intended to replace clinical judgment—it is intended to make the structure of that judgment visible, and thereby correctable.
| STAGE | CLINICAL QUESTIONS TO ASK EXPLICITLY | FAILURE MODE IF SKIPPED |
|
∅ I Neti Neti |
• Have I generated a differential that is broad enough to include diagnoses I have not yet seen in this patient? • Have I excluded the dangerous diagnoses first, regardless of their prior probability? • What evidence would falsify my leading hypothesis? Have I actively sought it? • Is my current front-runner surviving because it fits the evidence, or merely because I generated it first? |
Anchoring bias: the clinician commits to an early hypothesis and stops generating or testing alternatives. The correct diagnosis was never excluded; it was never considered. |
|
◈ II Viveka |
• Among surviving hypotheses, which fits the overall clinical pattern most coherently? • Am I weighting each feature appropriately, or am I over-indexing on a salient but non-specific finding? • What does Bayesian reasoning suggest given the pre-test probability and the sensitivity/specificity of the tests I have applied? • Does my pattern recognition align with or contradict the analytical evidence? |
Availability bias and premature closure: a recent memorable case, or an intuitively compelling pattern, displaces rigorous probabilistic discrimination among the survivors of Stage I. |
|
◎ III Prajñā |
• Does the analytically preferred diagnosis fit this particular patient’s context, values, and clinical trajectory? • What does my clinical experience with similar presentations suggest about the exceptions to the probabilistic rule? • Am I prepared to commit to a working diagnosis and act upon it, while remaining genuinely open to revision? • Have I communicated the basis and provisionality of this diagnosis to the patient and the team? |
Overconfidence and diagnostic momentum: having reached a provisional diagnosis, the clinician treats it as settled, fails to update on new information, and forecloses the very openness that prajñā requires. |
Applied Examples Across Clinical Presentations
The three-stage model applied to common high-stakes presentations
The following examples demonstrate how the three Medisophy stages apply to presentations encountered daily across emergency medicine, internal medicine, and primary care. Each case illustrates that the failure of a diagnosis to survive Stage I negation is not a failure of reasoning—it is reasoning succeeding.
| PRESENTATION | STAGE I — Negation | STAGE II — Discrimination | STAGE III — Wisdom |
|
Acute headache of sudden onset Emergency medicine |
Subarachnoid haemorrhage excluded first: lumbar puncture and CT interpretation interpreted in sequence. Meningitis excluded: absence of fever, photophobia, neck stiffness. | Pattern recognition of thunderclap onset weighed against prior migraine history. Probabilistic reasoning applied to age and vascular risk factors. | Working diagnosis of primary thunderclap headache enacted with explicit safety-netting: return precautions given, neurology follow-up arranged, provisional character of diagnosis communicated. |
|
Unexplained weight loss in a 65-year-old Internal medicine |
Malignancy excluded systematically by site-directed investigation. Thyrotoxicosis excluded by thyroid function testing. Occult infection excluded by inflammatory markers and targeted imaging. | Remaining hypotheses—depression, social isolation, medication effect—discriminated by structured history and collateral account from family. | Diagnosis of depressive disorder with social withdrawal enacted with sensitivity to patient’s reluctance to accept psychiatric framing; management plan adapted accordingly. |
|
Fatigue and low mood in a woman of reproductive age Primary care |
Hypothyroidism excluded by TSH measurement. Iron-deficiency anaemia excluded by full blood count and ferritin. Coeliac disease and inflammatory conditions excluded by targeted serological testing. | Depression and chronic fatigue syndrome discriminated through validated symptom scales, duration of symptoms, and functional impairment assessment. | Phronetic integration of the patient’s life context—recent bereavement, disrupted sleep, social withdrawal—informs a diagnosis of situational depression enacted with proportionate treatment and close follow-up. |
Integration with Clinical Decision Support Systems
Augmenting artificial intelligence with epistemic structure
The proliferation of clinical decision support systems (CDSS) and, more recently, large language model-based diagnostic assistants has created an urgent need for epistemic frameworks that can structure their outputs. The Medisophy model offers a principled template for this integration. Current CDSS tools are largely probabilistic engines: they rank diagnoses by likelihood. They do not, in their present form, distinguish between Stage I negation (has this diagnosis survived attempt at refutation?) and Stage II discrimination (among survivors, which fits the pattern most coherently?). This conflation produces a list, not a reasoning process.
The Medisophy Framework suggests three modifications to current CDSS design. First, systems should be architected to present Stage I outputs (mandatory exclusions by consequence) separately from Stage II outputs (probabilistic ranking among survivors). Second, CDSS alerts should flag when a high-consequence diagnosis has not been formally excluded, regardless of its rank-order probability. Third, and most significantly, Stage III—the integration of evidence with the particular patient—should remain explicitly outside the CDSS’s purview. The system’s role is to support Stages I and II. Stage III is the irreducibly human act of clinical judgment. This demarcation protects against both over-reliance on algorithmic outputs and under-utilisation of the tools’ genuine strengths.
Simulation-Based Training Applications
Using the framework to design and debrief clinical simulations
High-fidelity clinical simulation provides an environment in which the three Medisophy stages can be made explicit, observed, and debriefed without patient risk. The framework transforms simulation from a performance context into an epistemic training ground. Simulation scenarios should be designed with three corresponding phases: a breadth phase (Stage I), in which learners are required to generate and justify a differential before any investigation is ordered; a discrimination phase (Stage II), in which test results are released sequentially and learners are required to update their differential and articulate their probabilistic reasoning; and a commitment phase (Stage III), in which the clinical and contextual data are complete and the learner must enact a working diagnosis, communicate it, and defend its provisionality.
Debriefing structured around the Medisophy stages allows educators to name the specific epistemic failure that occurred. An anchoring error is a Stage I failure: the learner did not continue generating or testing alternatives. A premature closure error is a Stage II failure: the learner did not discriminate rigorously among the survivors. An overconfident diagnosis is a Stage III failure: the learner enacted a judgment without retaining the provisional openness that prajñā requires. This naming discipline is pedagogically powerful. When learners can locate their error within an epistemic framework, the corrective is conceptually clear: return to the stage that was inadequately executed.
Morbidity and Mortality Conference as Medisophy Audit
Reframing case review as retrospective epistemic analysis
The Morbidity and Mortality (M&M) conference is the most powerful existing structure for retrospective diagnostic learning in clinical medicine. Its current limitation is that it tends toward outcome-oriented analysis: what went wrong, and what was the result? The Medisophy Framework reorients M&M toward process-oriented analysis: at which epistemic stage did the reasoning fail, and why?
A Medisophy-structured M&M analysis asks three questions in sequence: Was the differential adequately broad at the outset, and were dangerous diagnoses excluded first? (Stage I audit.) Were the surviving hypotheses discriminated rigorously, or did a cognitive bias distort the weighting of evidence? (Stage II audit.) Was the enacted judgment appropriately provisional, was it communicated clearly, and was the team’s collective prajñā adequately cultivated to catch a revision signal when it emerged? (Stage III audit.) This sequenced analysis transforms the M&M conference from a retrospective account of error into a prospective training in epistemic discipline—a forum in which the logic of diagnosis is made visible, repeatable, and improvable.
REFERENCES
Scholarly Bibliography
Primary and secondary sources across all three traditions
CLINICAL REASONING & DIAGNOSTIC ERROR
1. Croskerry P. A universal model of diagnostic reasoning. Academic Medicine. 2002;77(6):547–553.
2. Croskerry P. Clinical cognition and diagnostic error: applications of a dual process model of reasoning. Advances in Health Sciences Education. 2009;14(Suppl 1):27–35.
3. Norman G. Dual processing and diagnostic errors. Advances in Health Sciences Education. 2009;14(Suppl 1):37–49.
4. Elstein AS, Schwartz A. Clinical problem solving and diagnostic decision making. BMJ. 2002;324(7339):729–732.
5. Kassirer JP. Teaching clinical reasoning: case-based and coached. Academic Medicine. 2010;85(7):1118–1124.
PHILOSOPHY OF SCIENCE
6. Popper KR. Logik der Forschung. Vienna: Julius Springer; 1934. [English trans.: The Logic of Scientific Discovery. London: Hutchinson; 1959.]
7. Kuhn TS. The Structure of Scientific Revolutions. Chicago: University of Chicago Press; 1962.
8. Lakatos I. The Methodology of Scientific Research Programmes. Cambridge: Cambridge University Press; 1978.
MATHEMATICAL LOGIC & FOUNDATIONS
9. Frege G. Begriffsschrift, eine der arithmetischen nachgebildete Formelsprache des reinen Denkens. Halle: Louis Nebert; 1879.
10. Russell B, Whitehead AN. Principia Mathematica. 3 vols. Cambridge: Cambridge University Press; 1910–1913.
11. Russell B. The Principles of Mathematics. Cambridge: Cambridge University Press; 1903.
VEDANTIC EPISTEMOLOGY & INDIAN PHILOSOPHY
12. Brihadaranyaka Upanishad. In: Olivelle P, trans. The Early Upanishads. New York: Oxford University Press; 1998.
13. Śṅkarācārya. Brahmasūtra-Bhāṣya. Gambhirananda S, trans. Kolkata: Advaita Ashrama; 1965.
14. Deutsch E. Advaita Vedānta: A Philosophical Reconstruction. Honolulu: University of Hawaii Press; 1969.
15. Mohanty JN. Reason and Tradition in Indian Thought. Oxford: Clarendon Press; 1992.
CLASSICAL PHILOSOPHY
16. Aristotle. Nicomachean Ethics. Ross WD, trans. Oxford: Oxford University Press; 1925. [esp. Book VI: Intellectual Virtue and phronēsis.]
17. Plato. Meno. Grube GMA, trans. Indianapolis: Hackett; 1976.
A framework developed by Dr. Abhijeet G. Shinde that integrates medicine, philosophy, and epistemology to understand clinical reasoning under uncertainty.












Leave a Reply